Persistent Pain
About Persistent or Chronic Pain
We hear about pain all the time, an advertisement for this, or there’s something about something else, but when it comes to Persistent or Chronic Pain, it’s a story that many ignore or dismiss as “isn’t happening”.
Approximately 3.4 million Australians cannot pretend it’s not there, and why? Because that’s about how many Australians are living with Persistent Pain.
Persistent pain is now considered a disease all on its own due to the impact it has, and the World Health Organization (WHO) has advanced recognition and treatment of persistent pain with two classifications: chronic primary pain and chronic secondary pain. “Primary” is used to describe a condition that is not caused by a different medical condition, while “secondary” means it is a consequence of another condition.
CHRONIC PRIMARY PAIN
- It is in one or more regions of the body.
- Persists for longer than three months
- It is associated with significant emotional distress or functional disability.
- Another chronic condition cannot explain it
CHRONIC SECONDARY PAIN
Chronic secondary pain is not a diagnosis on its own but instead an umbrella term for all the categories of nonprimary pain.
Presenting in numerous forms, Persistent Pain is typically considered to be pain that lasts for more than three months and simply means, on-going. Persistent pain occurs because of changes to the nerves or nervous system, often caused by a trauma of some description, which causes the nerves firing and signaling pain. However, there are likely to be other precipitating factors with Persistent Pain including genetics, gender and previous episodes of acute pain. If not managed well Persistent Pain can lead to various degrees of disability.
Apart from the well-documented cost Persistent Pain has on the economy and workforce, Persistent Pain can also create an enormous expense for the individual, their family, carers and loved ones; it is rarely only a financial one. The range of pain experiences is wide and varied. An individual’s response to persistent pain reflects characteristics of the pain and the person’s thoughts and behaviour developed during the course of the illness, which are subject to positive and negative reinforcement. The daily challenges of Persistent Pain that are commonly described include decreased enjoyment of normal activities, loss of function, role change and relationship difficulties. Uncertainty about ever being pain-free or the possibility of worsening pain is accompanied by feelings of anxiety, sadness, grief and anger. For some people, the burden of pain is difficult to manage and may lead to the emergence of a mental health disorder.
Major depression is the most common mental illness associated with Persistent Pain. High rates of generalised anxiety disorder, post-traumatic stress disorder and substance misuse have also been described. The lifetime prevalence of major depression in Australia is 11.6%, but it is 1.6 times higher in those reporting arthritis. In Canada, the prevalence of depression is three times greater in those with chronic back pain. In patients with Persistent Pain presenting for treatment, the prevalence of major depression is 30%–40%. [SOURCE]
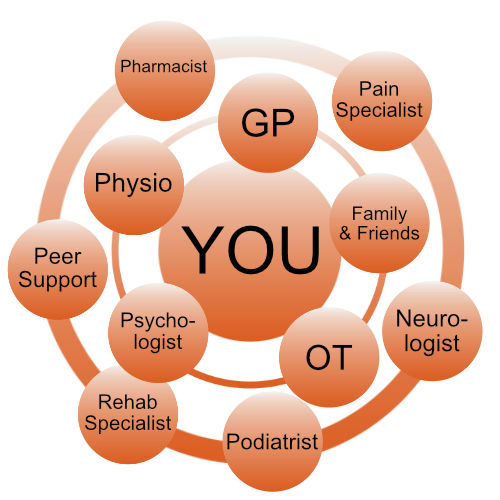
Like CRPS, Persistent Pain requires a multidisciplinary treatment approach, aiming to not only reduce pain, but increase movement and also improve quality of life.
Your treatment team will consist of doctors, specialists and allied health professionals.
If you need assistance finding a health professional in your area, you may find Painaustralia’s Pain Directory helpful.
Other helpful links
https://brainfoundation.org.au/disorders/dystonia
http://www.communitywebs.org/fibromyalgia/
https://www.msaustralia.org.au/
https://arthritisaustralia.com.au/
https://endometriosisaustralia.org/
https://www.diabetesaustralia.com.au/
https://chronicpainaustralia.org.au/
PainLink Helpline – 1300 340 357
Hidden Disabilities Sunflower
“Making the invisible visible
As diverse as these conditions are, so are your individual access needs and the barriers you face in your daily life. So you can opt to wear the Sunflower to discreetly be seen in shops, at work, on transport, or in public spaces.”
“Just because you can’t see it, doesn’t mean it is not there
Globally 1 in 7 of us live with a disability. That is approximately 1.3 billion people.
But while some of us experience a disability that is visible, many have a non-visible condition or experience a combination of both visible and non-visible conditions. These disabilities can be temporary, situational or permanent. They can be neurological, cognitive and neurodevelopmental as well as physical, visual, auditory and include sensory and processing difficulties. They can also be respiratory as well as chronic health conditions such as arthritis and diabetes, chronic pain and sleep disorders.”
become a member!
